Any type of joint disease occurs with degenerative and dystrophic processes in the joint tissue. This disease is always chronic in nature and cannot be completely cured, you can only slow down or stop its progression.
According to the ICD-10, gonarthrosis (injury to the knee joint) belongs to the group with the code "M17". The focus in treatment is on drug therapy, surgical intervention is used only when the course has advanced.
Knee joint is dry, what to do?
Knee osteoarthritis is accompanied by degenerative and dystrophic processes, which, if untreated, will progress stably. In this case, inflammatory processes are not observed, except in rare cases.
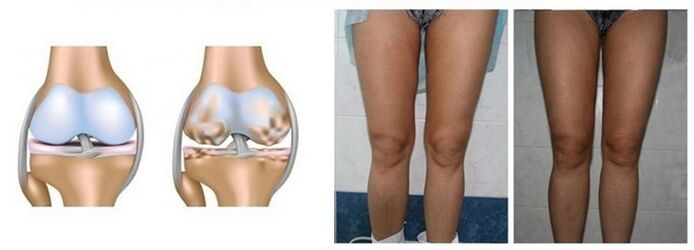
Degeneration and dystrophy of the joints at first practically do not affect the function of the knee. Over time, these processes lead to a violation of the structure of the joint, it stops "slipping", bumps appear on its surface (due to deforming changes).
Blood circulation is reduced, local metabolism (metabolism) is impaired, which only accelerates the progression of the disease. The degenerative process of hyaline cartilage begins very quickly, gradually thins, stratifies, and then cracks appear on it.
The end result of the disease is complete destruction (destruction) of the hyaline cartilage with adjacent bone contact. But the problem doesn't end there: as the bone is exposed, the back begins to thicken and bone over it (usually in the form of spines).
All of this also leads to deformity of the affected limb, which in turn leads to its curvature. It is for that reason that this disease is also known as "deforming joint disease". With a limb already deformed, the disease cannot be cured without surgery.
The reasons for the development of the disease
Often, the development of OA of the knee precedes the appearance of some causative factor. Congenital risk factors are not necessarily present, the disease very often develops with acquired factors (trauma, infection, inflammation).
Main reason:
- Severe disorders of metabolic / metabolic processes in the body (any acute or chronic severe disease of the thyroid, adrenal glands).
- Circulatory disturbances and a tendency to capillary bleeding (due to their fragility).
- Overweight (stage II-III obesity) with a severe increase in the load on the entire musculoskeletal system.
- Knee injuries (including direct trauma, penetrating wounds, ligament ruptures, meniscus injuries, fractures, dislocations and dislocations, and fractures).
- Inflammatory diseases in the recent past (primarily arthritis or rheumatism).
- Excessive physical activity (risk groups include athletes, exercisers, tennis, football, and basketball players).
- The consequences of a long-term knee injury are not completely treated.
- Congenital anomalies and anomalies in the structure of joint tissues, genetic risk factors (gene mutations).
There is a direct link between the cause and severity of joint disease. If metabolic disorders or severe trauma are the cause, the prognosis is worse than in the case of joint development due to joint overload or age-related dystrophic changes.
Rate statistics
Statistically, dry joint disease of the knee joint is very common, it occupies one of the leading positions among all forms of joint diseases in general. About 20% of patients who apply to specialized medical facilities have gonarthrosis.
If we consider all diseases of the knee joint, among them, the rate of joint disease falls in about 53% of cases. Recently, the number of cases of gonarthrosis in the population is increasing, especially in developed countries.
This is associated with an increase in life expectancy (the older a person is, the higher the risk of developing this form of joint disease), and with a predominance of a sedentary lifestyle. And this is a real problem, because doctors still haven't been able to completely cure gonarthrosis.
Why is gonarthrosis dangerous?
The main risk of gonarthrosis is disability due to the development of complications that cannot be treated with conservative therapy. First of all, this is a deformity of the bones and joints of the affected limb. Disability can occur in the third stage of the disease.
The second danger is the development of chronic severe pain, which can make the patient so uncomfortable that it is impossible to sleep normally. Constant awakening due to knee pain is one of the most common problems of stage 3-4 of gonarthrosis.
The lethal consequences are precisely because gonarthrosis does not arise. In theory, a serious injury could result from a sudden entrapment of a joint. This is a symptom known as joint blockade, which is usually observed in stages 3-4 of the disease.
Degree of gonarthrosis and the difference between them
The disease is divided into four stages, which differ in the severity of the course, the severity and number of symptoms, and the final prognosis. In addition, each stage of joint disease is treated in a unique way (although differences in treatment regimens may seem small to non-physicians).
Degree of gonarthrosis:
- First degree: the disease has practically no outward appearance, only mild discomfort, but in general the patient feels well and therefore it is difficult to diagnose the disease in the early stages;
- second degree: the appearance of severe pain, especially after walking or standing for a long time; characteristic crackles develop during physical activity, quadriceps atrophy may have already begun;
- The third degree: the pain becomes severe, constantly bothers the patient, there are obvious deforming changes in the joints, hot to the touch, normal walking or even being unable to run;
- grade 4: very difficult with severe deformities of the joints and constant pain that does not even allow the patient to sleep; Joint dysfunction is so pronounced that ankle sprains (complete immobilization of the affected joint) can occur.
The first two degrees of gonarthrosis are considered favorable, since they practically do not interfere with a person's normal life. The last two stages of the disease are very severe and lead to disability.
Symptoms of gonarthrosis at different stages
The clinical picture of gonarthrosis depends on the stage of the disease. In the early stages, there may be no symptoms, while in the fourth stage they are very pronounced and do not stop bothering the patient even with strong drug therapy.
Stage 1 symptoms:
- Discomfort or mild pain with severe stress on the joint.
- Almost unnoticeable.
- Subtly increase the size of the joint.
Stage 2 symptoms:
- pain of moderate intensity, often with a period of exacerbation and remission;
- joints become warm to the touch;
- there may be redness of the skin over the affected joint;
- moderate knee dysfunction (can still walk and run, but with some difficulty);
- Pain increases in the morning and after a long time in a standing position.
Stage 3 symptoms:
- severe pain bothers the patient around the clock, but during exacerbations (the onset of an exacerbation is individual to the patient), the pain increases several times;
- visible deforming changes in the knee, an increase in its size;
- the affected joint becomes hot to palpation;
- normal movement is impossible due to partial immobilization of the joint;
- legs can be bent.
Stage 4 symptoms:
- the pain becomes so severe that it does not allow the patient to do everyday things (including mental ones, because the pain impairs cognitive function);
- the appearance of synovitis due to the accumulation of effusion in the cavity of the cartilage of the knee;
- now deforming changes are clearly seen not only in the joint, but also in the whole limb;
- fluttering sensation when palpating the kneecap and surrounding tissues;
- almost complete or even complete immobilization of the knee joint (in this case only surgery can restore function of the limb).
If pain cannot be eliminated or significantly reduced at 3-4 stages of the degenerative joint process, doctors will resort to blocking analgesics, but this cannot be done on a daily basis.
Diagnose
The focus in diagnosing knee effusion is on imaging techniques, while laboratory tests often show nothing.
The diagnostic methods used are:
- Examination by an orthopedist with palpation of the affected joint, bone linearity measurement, vascular measurement.
- Clinical blood tests (total and erythrocyte sedimentation/ESR), determination of fibrinogen levels in blood and urine and, above all, urea, as well as other biochemical parameters.
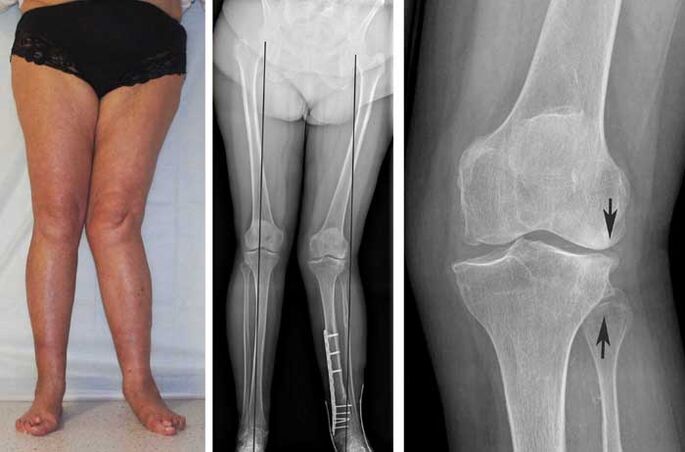
- X-rays (joint space narrowing, deformities, hardening of the cartilage, salt accumulation and even bone-forming substances are detected).
- Ultrasound examination (for differential diagnosis only).
- Magnetic resonance imaging or computed tomography (most informative, on imaging methods).
Usually, an X-ray is enough to make a diagnosis, especially if the disease is advanced. In relatively rare cases, computed tomography or magnetic resonance imaging is required.
Treatment of gonarthrosis: methods
Treatment of knee effusion is only complicated because there is no single treatment that is separate from the others that work well (even medication). The course of treatment is long, can last for years, and is sometimes prescribed for the rest of your life.
Treatments used:
- drug therapy - the basis of treatment;
- physical therapy exercises;
- dietary therapy;
- physiotherapeutic treatment;
- surgical intervention.
The main thing in the treatment of rheumatic diseases is the systematicity of the process and compliance with the recommendations of the attending physician. Attempts to independently treat gonarthrosis, including bypassing the doctor's prescription, often end in disability.
Exercise therapy
Physical therapy exercises are most suitable for treating stage 1-2 knee osteoarthritis. At such stages, this is pretty much the mainstay of treatment, as exercise can slow the progression of the disease and eliminate most symptoms.
However, without special meaning from classical physical education, it can also be harmful. Therefore, the patient is assigned special and individual exercises (since gonarthrosis can progress differently in each patient).
There is no time frame for treatment with therapeutic exercise methods - ideally, you'll need to engage in prescribed exercises for the rest of your life, seeing your doctor occasionally to monitor joint health. It is helpful to combine exercise therapy with exercises in the pool (where the load on the joints is much less).
Diet
Although nutritional modification can be very helpful, it is not a mandatory treatment. In only 40% of cases, dietary therapy produces noticeable results, and often in those with an endocrine-disrupting onset of joint disease.
Patients are instructed to give up fatty, fried, salty and smoked foods. A ban is put in place for the use of alcoholic beverages, sometimes smoking is also prohibited. At the same time, the consumption of large quantities of vegetables, fruits and meat products is regulated.
In this case, sausages, sausages or desiccants cannot be called meat products. Patients are instructed to consume lean meat, and boiled chicken is particularly helpful (due to its relatively low calorie content and high protein content).
Physical therapy
Physical therapy procedures are only helpful in relieving the symptoms of joint disease, but they do not directly affect the disease. That is, it is impossible to cure even the early stages of joint disease with the help of physical therapy, regardless of what some "specialists" say there.
Physical therapy is great for pain relief, but only if it is mild. With severe pain (stage 3-4 of joint disease), physical therapy will not help, as will most medications (especially oral).
The most preferred treatments for joint disease are magnetic therapy, quantum therapy, mud therapy, acupuncture, and hirudotherapy. Shock physiotherapy techniques are prohibited due to the risk of further joint damage.
Work
Only surgical intervention is required at stage 3-4 of the disease, when conservative methods are no longer necessary. Different types of procedures may be used: drainage of the joint cavity, removal of bone-forming material, joint (prosthetic) replacement.
To restore the function of the joint, it is best to implant it, but the problem is that this is a very expensive procedure. As a result, only 10-15% of patients can afford such a surgery. But even with the required amount, it is not always possible to replace the joint.
The fact is that such a procedure is contraindicated in patients with severe conditions, or in patients over 65-70 years old. Remember that any knee surgery carries its own risks of complications (even fatal complications can occur but are rare).
Medicine
Along with physiotherapeutic exercises is the basis of treatment and its obligatory component. If it is still not possible to apply other procedures, it cannot be treated with drugs in combination with exercise therapy (traditional medicine cannot replace drug treatment).
The patient is prescribed analgesics (in case of severe pain - blockade), decongestants, muscle relaxants, antihistamines. Chondroprotectors are often prescribed, possibly injecting hyaluronic acid (which replaces the physiological lubricant of the joints).
Drugs can actually affect the disease only in stages 1-2 of joint disease. In stages 3-4 of the disease, drug treatment acts only as a way to deal with the symptoms, while nothing but a surgery can affect the disease.
The nuances of treatment in the period of exacerbation and remission
Approaches to treating knee disease in exacerbation and remission are somewhat different. In the exacerbation phase, aggressive therapy is used, aimed at the fastest possible restoration of joint function and the elimination of symptoms.
The pain reaches its peak precisely at the exacerbation stage of the disease, therefore, in such cases, a blocker may be prescribed.
Non-steroidal anti-inflammatory drugs may be prescribed. Despite the fact that joint disease often progresses without inflammation, it can occur in the acute phase. Patients are prescribed bed rest, minimizing stress on the affected joint and avoiding overheating of the limbs.
In contrast, during the remission phase, physical exercises are prescribed and, in general, an increase in physical activity is prescribed. This is because you are in remission, so you can walk normally, because joint function improves and the pain is usually of moderate intensity.
It is necessary to use remission skillfully - this is the period when it is possible to do classes in the swimming pool, classes with a rehabilitation therapist and try to restore joint function. You cannot do without medication during this period.
Most often, chondroprotectors, oral analgesics are prescribed (at the discretion of the patient, since if the pain is insignificant, there is no need to take the drug). Ointments, gels and creams can be prescribed, including those with a warming effect (it is better not to use them during an exacerbation).
In addition, massage can be prescribed, including manual therapy (only if the disease is at stage 1-2). With the doctor's permission, special gymnastics techniques may be used.
Remission is an ideal time for physical therapy, but the choice of specific physiotherapy should be made by the physician, not the patient. Finally, if necessary, during remission, injections of hyaluronic acid preparations can be made.
With an exacerbation of arthritis, hyaluronic acid is not prescribed, because against inflammation, such an injection will lead to serious consequences. Please note: injections should only be administered by suitably qualified personnel.
Ordinary doctors, and even more so, mid-level medical personnel (medical staff, nurses), are not allowed to perform such injections. Self-injection into the joint is not only disabling but also fatal (due to the risk of anaphylaxis or blood clots if the needle accidentally enters a blood vessel).
Treatment prognosis
The prognosis for treatment of gonarthrosis varies depending on the stage of the disease and the general health of the patient. If this is stage 1-2 and treated immediately, the prognosis is very good, especially in people of working age.
With stage 3-4 osteoarthritis, the prognosis is extremely poor, in both young and elderly patients. Although it has been found that young people suffer from arthritis much more easily at such stages, it still inevitably leads to disability.
However, having stage 3-4 arthritis does not equate to a verdict. In fact, with the help of surgical intervention, you can try to restore, if not all of the function of the knee, most. Artificial joint implants can provide a great outcome.
Prevention of dry joints of the knee joint
Arthritis is a group of diseases that are completely preventable with fairly simple preventive measures. Of course, such measures do not guarantee 100% protection, but they can reduce the risk of disease (especially in those at risk).
Precautions:
- Unnecessary stress on the joints should be avoided (those loads include professional sports).
- Proper nutrition, mainly fruits and vegetables in daily meals.
- Keep fit and exercise regularly.
- Prevent or eliminate obesity (more body mass - more stress on joints in the body).
- Prophylactic treatment with chondroprotectors after the age of 45 years (only after consulting a doctor).
- Add enough fluids daily (about 1. 5 liters of water per day), limit salty foods.
The most important thing is not to overdo it with physical activities, since it is only useful in moderation (if the musculoskeletal system is not worn out). Sports are useful, sports are not, especially for bones and joints and the cardiovascular system.
























